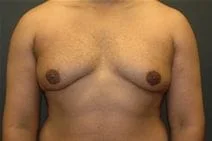
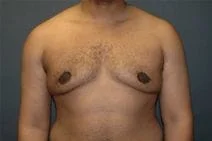
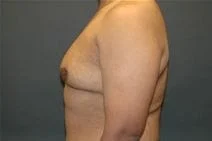
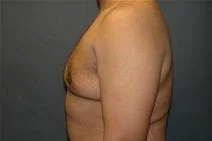
Gynecomastia is embarrassing feminine-appearing breast enlargement among male adolescents and adults alike. For adolescents, it can be a transient result of the changing hormonal milieu during puberty, and fortunately the majority of these cases regress spontaneously. For adult men, gynecomastia can be the result of weight gain or anabolic steroid use. There is a list of drugs and medications that can induce gynecomastia including marijuana, alcohol, antipsychotics and spironolactone.
For the majority of patients, gynecomastia is idiopathic, meaning there is no specific defining cause. For adolescents with significant gynecomastia, Dr. Lindsey requests consultation from the pediatrician to assure that the timing and planning of gynecomastia excision are appropriate. For adults, Dr. Lindsey will sometimes ask for medical clearance to assure there are no underlying causes that should be addressed first.
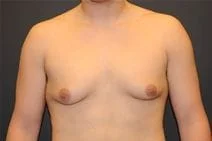
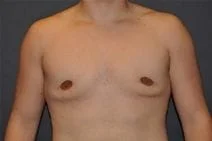
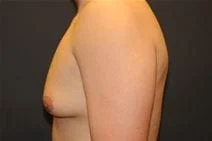
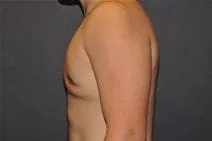
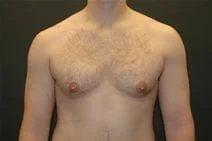
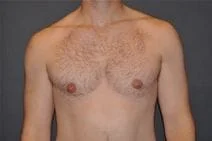
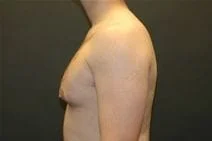
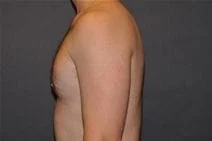
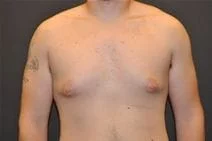
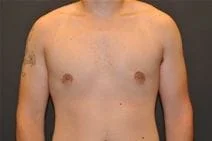
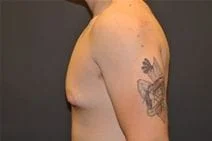
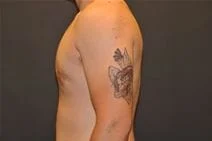
Removal of gynecomastia is very satisfying, as the surgical results are essentially immediate, and the resulting masculinization of the male chest quite evident. For small to moderate degrees of gynecomastia, the incision around part of the areola (periareolar) is all that is required with or without feathering circumferential liposuction as dictated by the anatomy. This is a particularly advantageous situation, as periareolar scars are typically almost invisible, allowing removal of the undesired female-like breast tissue in an almost scarless manner.
For severe gynecomastia, a different approach is required. This is typically an incision in the inframammary fold to remove all unwanted breast skin and breast followed by free nipple grafting, where the nipple is replaced as a free skin graft.
Gynecomastia excision is a significant surgery. The surgery recovery is typically low-pain and easy; however, it is major surgery, and activity limitations stay in effect for 6 weeks postoperatively. Surgical drains are sometimes used, depending on the size of the breast, but are usually removed within a few days of surgery. Dr. Lindsey advises compression of the chest area with two 6 inch Ace wraps or a custom-fit compression vest for a minimum of 2-3 weeks after surgery before graduating to a lightweight undergarment such as Underarmour.
Please view before and after photos of patients who have undergone removal of gynecomastia on this website to see if this procedure might be right for you.